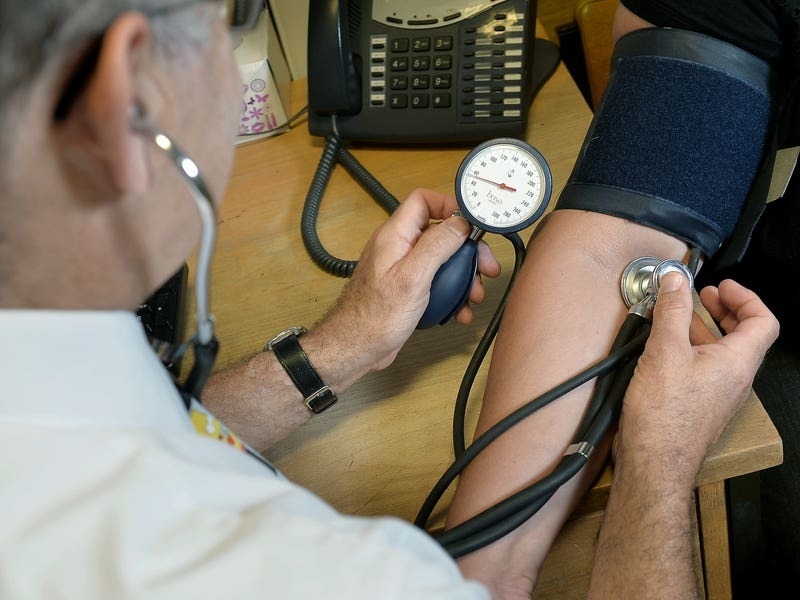
Seeing the same GP improves patient health and reduces the workload for family doctors, according to one of the largest studies of its kind.
Researchers at the University of Cambridge and INSEAD business school found there was a range of benefits when patients have a long-term relationship with their doctor.
Seeing the same doctor during GP visits – a model known as continuity of care – meant people waited on average 18% longer between visits, compared with patients who saw different doctors.
People did not take up more GP time in each consultation and the findings were particularly strong for older patients, those with multiple chronic illnesses, and people with mental health conditions.
They added: “Importantly, if patients receiving care from their regular doctors have longer intervals between consultations without requiring longer consultations, then continuity of care can potentially allow physicians to expand their patient list without increasing their time commitment.”
For the study, published in the journal Management Science and shared with the PA news agency, experts analysed more than 10 million GP consultations in 381 practices in England over a period of 11 years.
The study noted that: “A physician can be considered more productive if they improve the quality of care provided without reducing the number of patients they serve per year or if they serve more patients without reducing quality of care.
“If physicians provide high-quality care to their regular patients, they are likely to keep them healthier, which reduces the demand for consultations and increases their capacity to serve more patients.”
Co-author Professor Stefan Scholtes, from Cambridge Judge Business School, said seeing the same doctor could have substantial benefits, equivalent to increasing the GP workforce by 5%.
He said that “getting it right the first time” will reduce future workloads by “preventing revisits”, adding: “Better health translates into less demand for future consultations. Prioritising continuity of care is crucial in enhancing productivity.”
For the study, researchers used anonymised data from the Clinical Practice Research Datalink, consisting of more than 10 million GP visits between January 1, 2007 and December 31, 2017.
Dr Harshita Kajaria-Montag, lead author of the new study, who is now based at the Kelley School of Business at Indiana University in the US, said: “The benefits of continuity of care are obvious from a relationship point of view.
“If you’re a patient with complex health needs, you don’t want to have to explain your whole health history at every appointment.
“If you have a regular doctor who’s familiar with your history, it’s a far more efficient use of time, for doctor and patient.”
Analysis of England’s GP Patient Survey data by the Nuffield Trust shows that when asked ‘how often do you see or speak to your preferred GP when you would like to?’, there has been a decline in continuity of care over time.
Between 2018 and 2023, the proportion of patients who ‘always or almost always’ saw or spoke to their preferred GP decreased from 26% to 16% while those who answered ‘never or almost never’ increased from 10% to 19%.
Dr Victoria Tzortziou-Brown, vice chairwoman of the Royal College of GPs, said: “Continuity of care is highly valued by GPs and patients alike.
“We already know it is beneficial for patients, particularly those with complex health needs, and we know it has benefits for the NHS – and it’s encouraging to see that this study has found it can also improve GP workload. Studies such as this one are very important for informing future policy and practice.
“Currently, the intense workload and workforce pressures GPs are facing – as well as political agendas prioritising speedy access to GP services above all else – greatly limit the level of continuity we can offer.
“The average number of patients per fully qualified GP is now 2,294, meaning each GP is, on average, responsible for 260 more patients than they were six years ago.
“This is unsustainable and makes guaranteed access to the same GP for every patient practically impossible. However, it would be important that continuity of care is prioritised for those who need it the most.
“Before we can offer greater levels of continuity, we need to address the clear gaps in our workforce – we’ve lost 642 fully qualified, full-time GPs in the past five years – and provide support for the myriad of other challenges the profession faces including the rising rates of patients presenting with chronic, complex health conditions.”
An NHS spokesperson said: “Continuity of care with a GP or health professional familiar with a person’s care can be really important, but with record demand for services it can be difficult for practices to offer this for every patient.
“The NHS Long Term Workforce Plan offers a vital opportunity to grow the primary care workforce to meet increased demand, including increasing GP training places by 50%, to support general practice teams to provide continuity of care, especially for those who need it most such as older people or those with complex health needs.”
A Department of Health and Social Care spokesperson said: “Continuity of care is important, alongside speed and convenience of access. All patients must be assigned a named GP, and practices must endeavour to comply with all reasonable requests from patients to see a particular GP or other healthcare professional.”